What is Acne?
Acne happens when pores become clogged by dead skin cells resulting in build up of sebum, a greasy and waxy material made by oil glands.
Bacteria within pores, called Cutibacterium acnes (C. acnes), can contribute to pore blockage and inflammation – visible as redness, swelling and pus that may accompany acne spots. Cutibacterium can also make more dead skin cells accumulate. The result is acne, the term used to describe emerging blackheads, whiteheads, pimples and cysts.
Risk Factors
Everyone gets a pimple sometime in their life. Acne often starts around puberty and may last 5-10 years or continue into adulthood.
Causes
Around puberty, hormones lead to a combination of overactive sebaceous (oil-producing) glands that produce more sebum, and an increase in cells that block oil pores. This leads to the inflammation (redness and swelling) of acne.
Heredity (genes) is another factor determining who gets acne, and how severely. If either or both of your parents had acne you are more likely to develop acne too.
Triggers
Several factors can make acne flare up or lead to breakouts, but the triggers can vary from person to person. Every person is different. You can help to control the condition by avoiding things that you notice make your acne worse.
Cosmetics
Makeup and hair care products can clog pores. The Canadian Dermatology Association’s Skin Health Program recognizes skincare products that meet important criteria including being gentle on skin, fragrance-free and non-pore clogging. When shopping, look for our recognized product logo on labels. Other acne-friendly terms on labels to look for are ‘oil-free’, ‘non-comedogenic’ or ‘non-acnegenic’. Please visit our Skin Protection Program page to learn more or see the list of recognized products.
Physical pressure
Pressure due to a chinstrap, phone receiver, sports helmet, headband, guitar strap, bra strap, shoulder pads and other tight clothing can lead to acne developing at the point of skin contact.
Sweating
Excessive sweat can worsen acne in some people, especially if trapped under damp clothing.
Overwashing
Washing your face once or twice a day with a gentle cleanser is recommended for acne-prone skin. Cleaning it more often, scrubbing/exfoliating or using strong cleansers or astringent products (i.e. toners with alcohol) can irritate the skin and even worsen acne.
Medications
Certain medications can cause acne to flare up, such as oral corticosteroids, some contraceptives (progestin only) and anticonvulsants.
Menstrual cycle
Typically, many people notice that acne flares up in time with their monthly period cycle.
Picking or squeezing
Picking and squeezing acne spots can make them worse and increase risk of permanent scarring. This is because touching can push sebum and bacteria into surrounding skin tissues, leading to more swelling, redness and possible infection. This worsens the scarring.
Food
If a certain kind of food seems to aggravate your acne, avoid it. You may wish to avoid dairy products or adopt a diet with a low glycemic index as it could reduce symptoms for some people.
Stages of acne
Many terms are used to describe different types of acne such as:
Comedones – An open comedone is a blackhead, a closed comedone is a whitehead.
Papules – A red bump.
Pustules – A red bump with pus in it.
*Papules and pustules are often called pimples or zits.
Nodules – Located deeper under the skin.
Cysts – Located deeper under the skin and has pus in it.
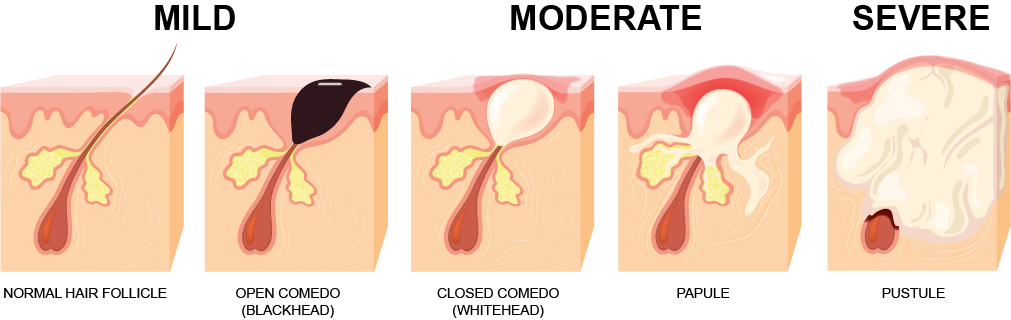
There are three levels of acne severity:
Mild — a few small lesions that are close to skin surface, may or may not be inflamed.
Moderate — marked by somewhat larger and more extensive whiteheads/blackheads and inflamed red spots that cover more of the face, possibly also on back and chest.
Severe — involves many more acne spots, some deeper lumps called nodules and cysts, redness and inflammation over much of the face and/or back and chest.
Acne by Age Group
Adult Acne
Acne that starts during adolescence may continue into adulthood, in milder or more severe form. Acne can begin in adulthood, too; three-quarters of adult acne occurs in women.
Hormone fluctuations are usually responsible, which is why some women may suffer ‘cyclical acne’ that shows up before menstrual periods, or flare-ups during pregnancy or menopause.
Adolescent Acne
Most teens are affected by acne to some degree. That’s because the surge in hormones that happens at puberty seems to jump-start acne. Everyone gets a pimple at some time and 9 in 10 adolescents will develop acne to some degree. Acne usually starts around puberty due to hormonal changes and usually lasts about five years although it can sometimes continue into adulthood.
- More than 80% of acne sufferers are between the ages of 12 and 24.
- Acne affects the face in 99% of cases.
- About 25% of all teenagers will still have acne at age 25.
Baby Acne
Acne can show up as early as birth; this form is called acne neonatorum, ‘baby acne’. It affects about 20 per cent of all newborns, mainly on the cheeks and nose. Lesions appear as small, red bumps.
Baby acne usually appears two weeks after birth, and lasts from a few weeks to at least three months. The cause is maternal hormones that remain after delivery and stimulate the baby’s sebaceous glands. Those hormones cross the placenta, ultimately causing the overactive oil glands to produce pimple-like bumps.
Baby acne can flare up and become more irritated when skin comes into contact with saliva, milk, some fabrics or when the child is too hot. Unlike other acne types, baby acne clears up on its own and doesn’t require any treatment. In severe cases, a doctor may recommend some form of topical treatment. Having baby acne does not predict who will develop acne in adolescence.
Impact
Psychological Effects
While acne is very common it can still have a significant psychological impact and cause embarrassment and low self-esteem. It can interfere with daily activities and impair willingness to go out with friends, speaking in public, going to the pool, etc. When the impact is particularly severe it can lead to depression. Re-assurance and counseling are important along with early treatment to prevent these psychological effects.
A Canadian study of nearly 500 patients with acne, published in the British Journal of Dermatology, found that even having mild acne can evoke feelings of low self-esteem, depression and thoughts of self harm. The fact that acne often coincides with the start of puberty adds to feelings of uncertainty about self-image and can contribute to emotional issues.
Scarring
Even mild acne can cause scarring, although the more severe (cystic) acne is associated most strongly with scarring risk. The risk of scarring is highest in those with severe acne, those who have had acne for a prolonged time, those with a family history of acne scarring, and those who squeeze or manipulate their acne spots.
Scars result from injury to the skin. There are two types: atrophic (loss of tissue) or hypertrophic (greater amount of tissue) scars. These present as divots or indents due to loss of skin tissue or rubbery thickened knots of skin, respectively.
Facts
- Acne affects 5.6 million Canadians, nearly 20 per cent of the population.
- More than 80 per cent of acne sufferers are between ages 12 and 24.
- Acne affects about 90 per cent of adolescents, and 20-30 per cent of adults ages 20 to 40.
- Acne affects the face in 99 per cent of cases but can also affect the body in 50% of cases.
- Infant acne affects approximately 20 per cent of newborns.
- Starting around puberty and lasting until adulthood, acne can persist for many years, regardless of age.
- About 25 per cent of teens will still have acne at age 25.
- Women make up 75 per cent of adult cases.
Acne Myths
Eating greasy food makes acne worse — Certain foods such as chocolate, french fries and other greasy foods have long been suspected of aggravating acne, but scientific studies have not found a connection.
Poor hygiene can cause acne — Acne is not due to dirty skin, and doesn’t reflect personal hygiene habits. And blackheads aren’t dirt-filled pores. They’re black because the oil in them (keratin) is oxidized when it comes into contact with air. In fact, washing vigorously and too often can make acne worse by irritating the skin.
Acne will go away quickly — It may clear up, but acne can get worse before it improves. The longer you have acne, the greater the chances of permanent scarring. The most effective way to get rid of acne is to talk to your doctor about what treatment is right for you.
You can get acne from contact with someone who has it — Acne may be unsightly and embarrassing, but it is not contagious.
Sun exposure and tanning clear up skin — Neither outdoor nor indoor tanning will help acne over the long run. Being in the sun can seem to help initially by decreasing inflammation which may mask spots. But more often people will experience an acne flare-up after UV exposure. Tanning will make the brown or red spots left by acne more noticeable, and slower to fade . Sun exposure also raises the risk of skin cancer, increases wrinkles, and causes brown spots from ultraviolet damage to the skin.
Acne Do’s and Dont’s
Do wash your face! Cleanse with gentle cleanser once or twice daily.
Don’t over wash! It can irritate skin and aggravate your acne.
Do apply sunscreen! Skin is much more sensitive to UV rays when you use acne treatment products. Choose one that is non-comedogenic and non-acnegenic.
Do use oil-free products if you wear makeup. Look for non-comedogenic products – those that don’t contain pore-clogging ingredients.
Do launder pillowcases and sheets often. They absorb oil, and can lead to more deposition of dirt and oil on your skin.
Do wash makeup brushes with soap. Makeup applicators can store bacteria.
Don’t pop! Picking and squeezing worsens acne. It can also lead to more stains and scars.
Don’t stress out! Stress can indirectly worsen acne by affecting your hormones.
Don’t feel alone. Nearly everyone in the world gets pimples.
Treatment
Your doctor or a Certified Dermatologist can help with acne at any stage. Even mild acne can lead to scarring, and there’s no way to predict whether mild acne will progress to becoming more severe.
Non-prescription medications/Over-the-counter (OTC)
For mild acne, you can try OTC treatments before asking your doctor for help. These are usually milder than prescription-strength products, and are readily available in retails stores. Examples are medicated cleansers and topical creams and gels.
Active ingredients usually include salicylic acid or benzoyl peroxide. Salicylic acid boosts anti-inflammatory and peeling action while benzoyl peroxide kills bacteria and is known to cause drying and slight peeling. Benzoyl peroxide-based cleansers and creams are available OTC in concentrations of 5 per cent or less, or in higher concentrations (10 per cent) by prescription. Whatever you try, you need to stick to the treatment for a couple of months before seeing a difference. Visit your doctor if you don’t notice improvement within six to eight weeks.
Tips
- Topical medication should be applied to the entire affected area, not just individual pimples.
- Applying more won’t work better or faster, so apply a thin layer evenly.
- Use product as directed on the label and as recommended by your doctor.
- Products containing benzoyl peroxide can make your skin more sensitive to the sun, so reduce sun exposure and wear sun protection.
- Benzoyl peroxide bleaches sheets and clothing. Sleep in older pajamas and use an old pillowcase/towel.
- Apply your acne medication first, and let it dry before applying makeup.
- Keep using the treatment even after acne has visibly improved, to prevent new acne from forming.
Prescription medications
Prescription-strength acne treatments can include topical formulations, such as antibiotics, retinoids (vitamin A derivatives), benzoyl peroxide, anti-inflammatory medications (eg. dapsone and azelaic acid) and their fixed dose combinations. Oral (systemic) medication can include antibiotics, retinoids or hormonal agents (i.e. birth control pills, spironolactone).
Topical antibiotics (i.e. erythromycin, clindamycin) can be recommended to help control the inflammation associated with the redness and swelling of acne. These should be used in combination with benzoyl peroxide to prevent the development of antibiotic resistant bacteria.
Oral antibiotics (i.e. tetracycline, minocycline) are usually indicated for moderate to severe acne of the chest, back and shoulders. Treatment should be restricted to a few months to prevent antibiotic resistance developing. These should be used in combination with benzoyl peroxide for reasons stated above.
Hormonal agents such as oral contraceptives (OCs), topical clascoterone and spironolactone, are recommended for moderate to severe acne (e.g. cystic). They are often use in combination with topical treatments. Acne that flares up in the premenstrual part of the cycle and acne that occurs along the jawline, which is usually hormonal, both respond to hormonal therapy.
Retinoids (vitamin A derivatives) come in topical and oral forms.
Topical retinoids (i.e. tretinoin, adapalene, tazarotene, trifarotene) help reduce pore blockage and reduce inflammation. They are used across the spectrum of acne from mild to severe.
Oral isotretinoin is the only oral retinoid indicated for acne. It is reserved for severe acne or for cases not responding to the other treatments discussed.
Why stick with treatment?
Once your doctor has prescribed a treatment, you should use it properly and continue for as long as recommended. Many acne medications initially cause dryness, peeling, flaking, redness, irritation and/or possibly acne flare-ups. In some cases, acne can worsen before getting better. Any of these effects can lead some to stop treatment early. Ask and understand why your doctor prescribed a certain treatment, how to use it and for how long, what results to expect and when you should see improvement.
Your doctor may suggest easing into a treatment regimen to allow your skin to get used to it. For example, using the product every 2nd or 3rd night can reduce the risk of irritation. Moisturizer use can reduce dryness and scaling. After 2-4 weeks, your skin should be used to the product and you should be able to apply and leave it on all day/night without significant irritation. Any skin irritation due to treatment should subside after a few days of use.
Treatments to reduce scarring
Prevention is the best treatment: this includes treating acne early and controlling it to prevent new lesions forming. If you develop scars, ask a dermatologist about treatment options.
Retinoid creams and gels can be used to treat superficial scarring (not for deep or elevated scarring). They assist collagen production, helping skin to build new unscarred tissue.
Chemical or alphahydroxy acid (AHA) topicals and peels help smooth out slight discoloration, imperfections and improve skin tone.
Microdermabrasion, may help improve the uppermost damaged layers of skin.
Injectable fillers include materials such as hyaluronic acid, which are injected below the skin’s surface to plump up pitted areas.
Microneedling or laser skin resurfacing removes the damaged surface skin layer, which helps smooth out the appearance of deeper scars; it also encourages new collagen formation.
Subcision is when a needle is used to release the bound-down skin leading to some pitted scars. This and other treatments may be offered by your dermatologist.
Post-Inflammatory Hyperpigmentation
Post-inflammatory hyperpigmentation (PIH) can occur after your skin has been irritated or injured, and appears as patches or spots of darker skin.
Most PIH fades, but some that is deeper will not. Fading PIH can take many months to happen. Treatments for PIH could include: retinoids, alpha hydroxy acids, beta hydroxy acids, and azelaic acid (dicarboxylic acid).
Laser can be used for PIH, but those people who tan easily have higher risk of pigmentation and should only see some with expertise in this area who is used to working in such skin types.