What is Melanoma?
Malignant melanoma is a less common but highly dangerous skin cancer.
When found at an early stage, melanoma has one of the highest cure rates of all cancers, at more than 90 per cent. If left untreated, melanoma will invade the skin. When it reaches the bloodstream or the lymphatic system, it can spread to other parts of the body and often causes death.
Melanoma is a form of skin cancer. It starts in the melanocytes or pigment-producing cells in the outer layer of the skin. These cells grow out of control and form a tumour. Melanomas are often brown and black, but can also appear in other colours.
Types of Melanoma
There are four main types:
Superficial spreading melanoma accounts for about 70 per cent of cases. These lesions tend to grow outwards, so watch for spots or moles that are growing/spreading.
Nodular melanoma is a more dangerous form of melanoma since it grows quickly downward into the skin. It often appears on areas not usually exposed to the sun. It appears as a raised area and is usually very dark, but sometimes reddish.
Lentigo maligna melanoma appears on the parts of the body constantly exposed to direct sunlight. It is frequently found among older people. It often appears as a fairly wide, flat brown patch marked by several hues of brown and black.
Acral lentiginous melanoma is the most common melanoma in dark-skinned people and those of Asian descent. It appears on soles of feet, palms of hands and under toenails and fingernails.
Stages of Melanoma
There are five stages of melanoma based on the thickness and other features of the tumour. These stages provide an important guide to treatment, indicate the risk of recurrence and determine whether other tests are needed.
Stage 0
Melanoma in situ is the most frequent stage, when the tumour is limited to the outer layer of the skin and has not spread. Surgery is done to remove the melanoma and the surrounding skin, which completes the treatment. The prognosis is excellent.
Stage 1
These are very early melanomas. Depending on the severity, a sentinel lymph-node biopsy is sometimes suggested. Treatment also includes a local re-excision.
Stage 2
The tumour is more advanced and is deeper in the skin. A sentinel lymph-node biopsy is usually suggested. After surgery there is a moderate risk of recurrence or spread to another part of the body because of the depth of the tumour.
Stage 3
The melanoma has spread to nearby lymph nodes; these are removed in treatment.
Stage 4
This is an advanced stage of melanoma. The cancer has spread to another part of the body such as the lungs, liver, brain or abdomen. This situation is rare.
For Stages 3 and 4, post-surgical treatment focuses on preventing the cancer from coming back and on killing the cancer cells in the body. The following treatments, used alone or in combination, may be prescribed.
Chemotherapy
Chemotherapy drugs are often used to treat local recurrence, advanced melanoma that has spread or to control the symptoms of advanced melanoma. Side-effects can include nausea and vomiting, fatigue and hair loss. Chemotherapy can also increase the risk of infection for a time after treatment.
Biological therapy (or immunotherapy)
Biological therapy boosts the immune system to help the body act against cancer cells. These drugs target specific types of cells and, less frequently, damaged normal cells. Side-effects of biological therapy can include fatique, fever or chills, rashes or reactions at the injection site. Biological therapies used to treat melanoma include interferon and interleukin-2, ipilimumab, nivolumab and pembrolizumab
Targeted therapy
Targeted therapy involves treatment for patients whose melanoma has specific genetic changes such as a BRAFV600 mutation. Such mutations are found by testing samples of a patient’s tumour. The MEK gene works together with BRAF gene. MEK inhibitors help BRAF inhibitors to fight tumor cells. Currently approved targeted therapies in Canada include vemurafenib, dabrafenib and trametinib. Some side-effects of targeted therapy may include skin toxicities, fevers and chills, eye problems, diarrhea and heart problems. Several new targeted therapies are being evaluated in clinical trials.
Radiation therapy
Radiation therapy uses high energy x-rays or other types of radiation to kill cancer cells or stop them from growing. It is sometimes used after surgery to relieve or control symptoms, or to treat melanoma that has spread to the brain.
Radiation therapy damages both normal cells and cancer cells in its path. Side-effects depend on the area treated, and may include skin redness or irritation and fatigue. In stage III melanoma, radiation may be used after surgery to prevent spread and recurrence. In stage IV disease, radiation may help control symptoms.
5 Step Skin Cancer Self-Examination
While people may be unsure how best to check their skin, performing a self-examination using the steps below and the “ABCDEs” is a simple way to remember the key characteristics that could identify a potential case of melanoma.
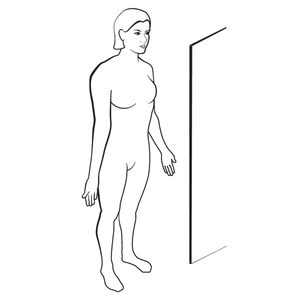
Using a mirror in a well-lit room, check the front of your body – face, neck, shoulders, arms, chest, abdomen, thighs and lower legs.
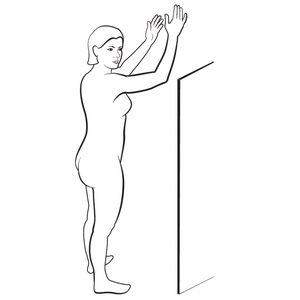
Turn sideways, raise your arms and look carefully at the right and left sides of your body, including the underarm area.
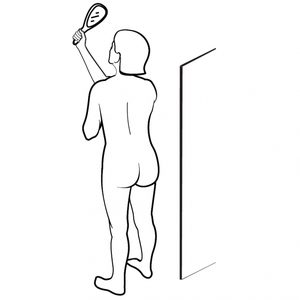
With a hand-held mirror, check your upper back, neck and scalp. Next, examine your lower back, buttocks, backs of thighs and calves.
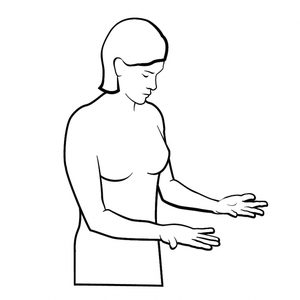
Examine your forearms, palms, back of the hands, fingernails and in between each finger.
Finally, check your feet – the tops, soles, toenails, toes and spaces in between.